Urology Treatments
Male Incontinence
It is a great number of men who silently, often with shame, suffer from urine leakage.
Male Incontinence
Table of Contents
DEFINItion
Incontinence in men? Yes, it has a solution.
Historically, the discomfort of incontinence has been commonly associated with the elderly, and more specifically the female gender. But Urology experts know very well that this is not entirely true. A considerable number of men suffer from this condition in silence, often with shame from the urine loss.
Today, thanks to the advanced materials we use in the operating room and the advanced surgical techniques we employ, we can affirm that male incontinence can be greatly reduced or eliminated in most cases.
From this article, you will get answers to the most frequently asked questions related to treatment with artificial sphincter or extrusion mesh, two of the most innovative solutions in the treatment of incontinence that make it possible to recover a comfortable and quiet life.
Looking for prices and information?
Use our virtual assistant and receive in your email everything related to the treatments that interest you. Budgets, recovery times, hospitalization, financing possibilities month by month, etc.
In just a few minutes and without any commitment.
En cumplimiento del Reglamento General de Protección de Datos le informamos que los datos por Vd. proporcionados serán objeto de tratamiento por parte de Andromedi con la finalidad de prestarle el servicio solicitado y/o contratado. Los datos no se cederán a terceros salvo en los casos en que exista una obligación legal. Para más información puede consultarla pinchando aquí.
Male Incontinence
Treatment Summary
This is short summary of the whole process: from the appointment request, to receiving the medical discharge after the treatment in some our Andromedi centers in Madrid, Seville or Canary islands (Tenerife)
Consultations Needed
The diagnosis of male incontinence only requires a medical consultation. Surgery will probably require a few more appointments to assess the situation.
Hospital Stay
It is necessary for the patient to remain in the clinic for 24 hours after surgery for some medical check-ups.
Anesthesia Type
Local, accompanied by mild sedation. The patient will remain asleep during the surgery but without being made unconscious by general anesthesia.
Operation Time
The intervention to solve the urinary incontinence in the male lasts between 30 and 45 minutes. It rarely exceeds one hour in the operating room.
Post-operative
Keep rest at home taking care not to make physical effort. About ten days will be necessary as well as much hydration and laxatives.
Resuming Sex Life
After about 10 to 15 days, the patient may be living a normal life. This includes sexual relations.
Frequent causes
What is Urine loss and what are its most common causes?
Urinary incontinence (UI) is defined as the accidental loss of urine. It is not a disease in itself but is rather an alert or an indication that there is a problem in the male urinary tract.
Urine (urination, or as it is commonly called; pee) is the main product of renal function. It is gradually stored in the muscular cavity that we know as the bladder, waiting to be emptied. The urinary sphincter is the entire area surrounding the urethra (outflow duct) and is responsible for controlling the discharge of stored urine with nerve impulses. It is this collaborative work between muscles and nerves that keeps the whole system in a healthy person without leaks, and also allows us to perform the discharge when we feel like peeing.
Any problem at some point in this organ chain most likely leads to UI. So, not all cases share the same origin. At Andromedi, we always study the specific causes of each patient in order to offer the most appropriate treatment.
At Andromedi, we always study the specific causes of each patient in order to offer the most appropriate treatment.
These causes can be of several types:
1 Problems related to the prostate: surgeries, cancer, etc.
2 Diabetes, Parkinson’s, Sclerosis or rare neuro-degenerative diseases
3 Problems derived from injuries in the urethra or bladder, or diseases related to these areas
Types of urinary incontinence
4 Stress-related incontinence: Often occurs alongside other functions of the body that involve some effort such as exercise, sneezing, coughing, laughter, etc.
5 Urge incontinence: This type occurs when the usual signal of needing to go to the bathroom is so sudden and so uncontrollable that it does not allow time to empty the urinary bladder in a controlled manner (and leaks occur).

Types of urinary incontinence

Types of urinary incontinence
6 Overflow incontinence: There are some patients who can not empty their bladder normally and later begin to suffer from an annoying drip.

Types of urinary incontinence
7 Suffering in silence: incontinence in men is more common than you think.
Mixed Incontinence which is usually of multiple origins presents with combined features of the other types.
UI is commonly associated with the elderly or people with aging symptoms. It is true that age is a risk factor that helps its appearance; however, we cannot directly establish that we must suffer urine loss as we grow older.
Approximately 15% to 20% of men over sixty suffer from urinary incontinence. Despite this large number, I have probably never heard many men admit to having this condition. It is not the type of illness widely regarded as an affliction or a mishap; UI is something that is kept in secret with embarrassment and shame. Even in our practice, patients when dealing with specialists who want to help them with their problems still appear withdrawn and embarrassed.
UI goes beyond physiological discomfort; it is something that often generates a psychological problem. The self-esteem of men who have to get to the point of using diapers is usually diminished. The image of confidence they had of themselves becomes less certain, with the perception that they will be harshly judged and ridiculed or mocked if others (men, but especially women) find out. The social patterns of manhood and masculinity are closely related to all this. Consequently, most of them end up locking themselves in without asking for help and not knowing that it is an ailment with a pretty effective surgical solution nowadays. (link)
All this, in patients with radical prostatectomy, who in large numbers also suffer from serious erection problems, involve a psychological handicap which they should not suffer in silence. Instead, it’s important that they seek the help and support of a professional.
In our offices in Madrid, Seville and the Canary Islands, we have amassed so much experience not only in the operating room implanting sphincters or artificial meshes, but have also developed our care and expertise after years of providing psychological assistance and companionship with maximum privacy and discretion to this type of patients. We perfectly understand what they are going through, their fears, their routines, their frustrations, and their discomfort. And that is why we can offer them comprehensive treatment. Fortunately, our satisfaction rate is also quite high because we deal with people and not with numbers from a row of people to operate. In a few years, there are people who go from feeling healthy to feeling old and broken.
Today thanks to the advancement of the materials that we use in the operating room and the advanced techniques of the operating room, we can affirm that male incontinence can be greatly reduced or totally eliminated in the vast majority of cases.
UI has a psychological component that we must not overlook. For example, work is an obvious cause of stress. Sex becomes very complicated and scary. Practicing sports or exercise tend to involve too much risk. The hours of sleep become unstable and you don’t get to rest properly. Many men end up arranging their lives and daily activities based on how far they will be from a urinal and then resort to leaving home very little, losing relationships and eventually wilting their lives in many ways because of this problem.
differences by sex
Differences between female and male incontinence
Both genders are definitely incomparable and comparing them is really not necessary because they have very different physiopathology. However, we see it relevant to further explain their differences:
Different causes
They are often caused by more “natural” causes such as pregnancy or menopause and they involve prostate problems (and surgical interventions) or neurological disorders.
Type of incontinence presented
While the most common cause of UI in females is stress, the so-called “overactive bladder” is the most common cause for men.

Male incontinence
Women suffer in greater numbers
Once again … the importance of leading a healthy lifestyle.

Female incontinence
Diet can have a diuretic effect on our body, and although there are foods that are generally more diuretic than others, each case is unique and should be studied in isolation. Foods that can be highlighted as being suspected of influencing UI may be alcohol, coffee, spicy, acidic, or sugary (soft drinks, chocolate, pastries). Patients will most likely experience improvement if they reduce one or more ingredients on this list from their diets.
One of the first “typical” temptations of people suffering from urine leakage is reducing the amount of liquid they drink to avoid problems. It is not recommended for the general health of the body, and particularly not recommended for the bladder, which can suffer complications when taking more concentrated urine capable of causing irritation in the urinary tract. Spacing out the fluid intake, while taking a healthy amount, can be an intermediate solution.
If stress plays an obvious role in a patient’s UI, a somewhat complicated and difficult though fruitful path may be to progressively train the body by introducing it into a routine that leads to better control of the sphincters. Through relaxation, meditation or conscious breathing, you can become more connected with your body to relieve and control the symptoms. Once a certain degree of self-knowledge has been reached, urinating with progressively ascending intervals (first every hour, then every hour and a half, etc.) can lead to a routine for the individual that reduces the number of leaks. As earlier mentioned, it is very laborious but can get good results.
Kegel exercises, erroneously reserved only for women, can be beneficial in increasing the muscle tone of the pelvic area to help the bladder retain urine more efficiently. We will not expand too much on this point because you can find many guides on the Internet that provide support in the performance of these routines

Diapers, a necessary tool before the intervention.
Many men are reluctant to use diapers because they find them directly humiliating. But while looking for a solution, as we will see later with surgical help, they are very useful, because, in addition to being capable of stopping the leaks, they protect the skin from probable irritation and prevent odors. The specific designs that exist for adults are far from what you might imagine. They are very discreet and specifically developed according to the daily routines of these types of patients.
Once that fear has been overcome, we can go into a little more detail, looking at the brand and the specific model which must be closely related to the specific symptoms. For severe urinary incontinence, the ideal option may be highly absorbent protective or disposable underwear. Individuals with milder symptoms may need less protection. Collectors are disposable quilted covers that go around the penis; They are good for light filtration or dripping. These pads which are designed for light or moderate leakage can be tucked into the underwear and are attached with adhesive tabs.
External catheters roll over the penis like condoms and trap urine. They are attached to drainage bags that can be hung on the side of your bed while you sleep or tied to the body under your clothes during the day.
As we said, all these solutions are ideally temporary. The most reliable and definitive new option is surgery.
solutions
Drugs and urine loss.

For men with urge incontinence, medications can help. Some relax the muscles to help prevent unwanted contractions of the bladder while others block the nerve signals to the bladder that cause it to contract at the wrong time. Medications prescribed to reduce the enlarged prostate may help with other urinary problems.
Always pay attention to the side effects of the medication. You should make sure that the medical team in charge of your treatment is aware of any interactions that the medicines and supplements you use possess which may affect your UI as there are many that can worsen the symptoms. Some antidepressants, sedatives, diuretics and even cold and allergy medications can enhance this problem.
Surgery is undoubtedly the most modern, safe and effective solution
Dr. Madurga, a member of the Andromedi team, is an expert in Spain and Europe in the surgical treatment of incontinence and is a great resource for the patients of our center, coming from all over the world. We consulted her to give us first-hand answers to the most frequently asked questions by patients in our Madrid, Seville and Tenerife offices.
Who are the candidates for this surgery?
100% of male patients who have urinary incontinence, regardless of the cause or nature may be candidates for this surgery. There are no factors that could make its implementation impossible. There is no age limit, as long as the pre-anesthetic tests are positive.
What is involved in the preparation for the surgery? What previous steps must be taken before it is performed?
After a first consultation and the indication of a sphincter implant or mesh, we perform an anamnesis (a general review of the patient’s entire clinical history), an examination of the area to be treated (to assess the degree of functionality of the urinary sphincter) and a urethrocystoscopy (to check the caliber of the urethra).
Why do we consider artificial sphincters and mesh? What are the differences and in which case do they apply?
Depending on the severity of the incontinence, different possible techniques are indicated. If there is a large amount of leakage, we opt for the urinary sphincter, and if it is moderate, we opt for the sub-urethral compression mesh. After the intervention, a patient who has been implanted with a sphincter must learn its management (urinating on demand by manipulation of the mechanism). Meanwhile, with the mesh, there is no need for manipulation. The material of the mesh is polypropylene while the sphincter is made of silicone. There are also price differences since the sub-urethral mesh treatment is cheaper than the sphincter treatment.
It should be noted that at Andromedi, we offer to combine both solutions with the dual surgery of penile prosthesis, which as we have mentioned above is usually indicated for patients and can be added to the dictionary as a solution to their added loss of erectile function.
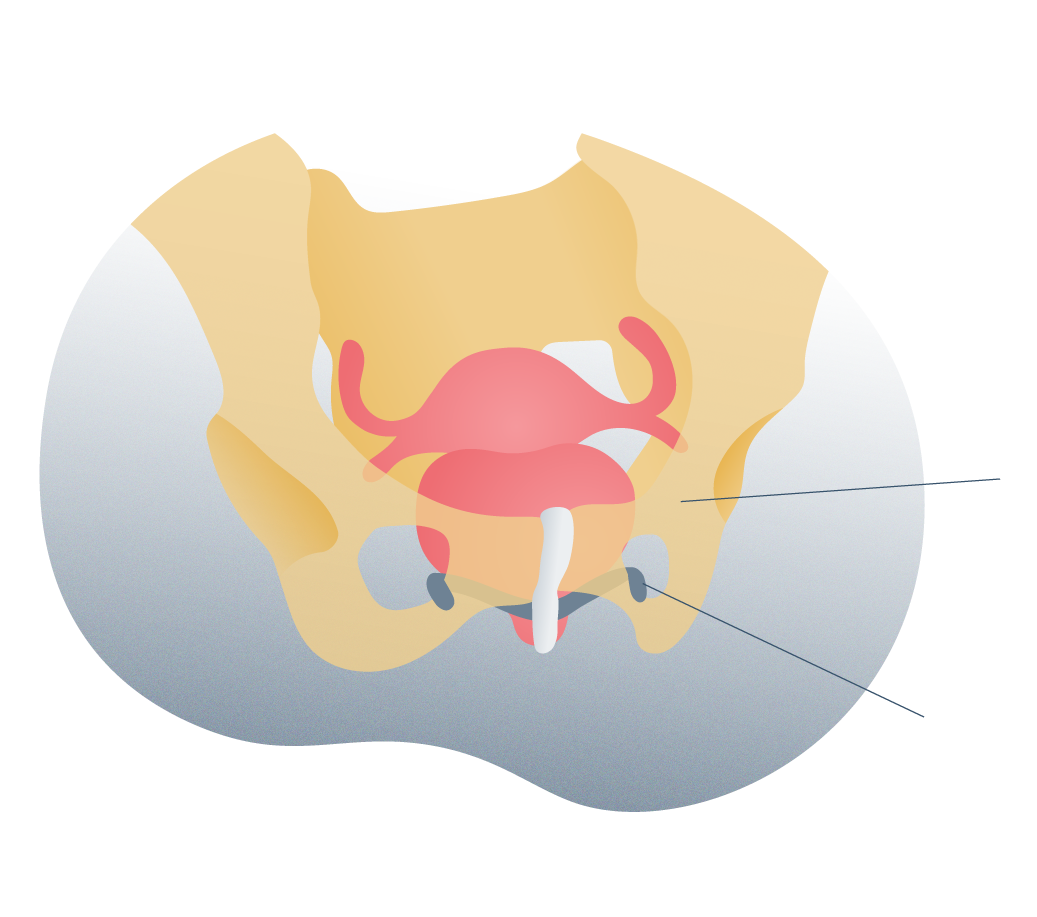
Male suburethral mesh surgery
OPINION
Real Testimonies from Our Patients in our Andromedi centres in Madrid, Seville and the Canary Islands.
JJ
Paciente de incontinencia
Author
Natalio Cruz MD, with 25 years of medical experience, has been until 2016 Head of the Andrology Unit in the Urology Service of the Virgen del Rocío Hospital in Seville, National Coordinator of Andrology in the Spanish Association of Urology (AEU) and General Secretary in the ESSM, positions that he has narrowed to focus squarely on this exciting project of offering a high-level private medical consultation in Marbella, Seville, Madrid and Tenerife.
Andromedi pertenece a las organizciones médicas más destacadas en el sector de la Uro-Andrología