symptomatology
Signs and symptoms
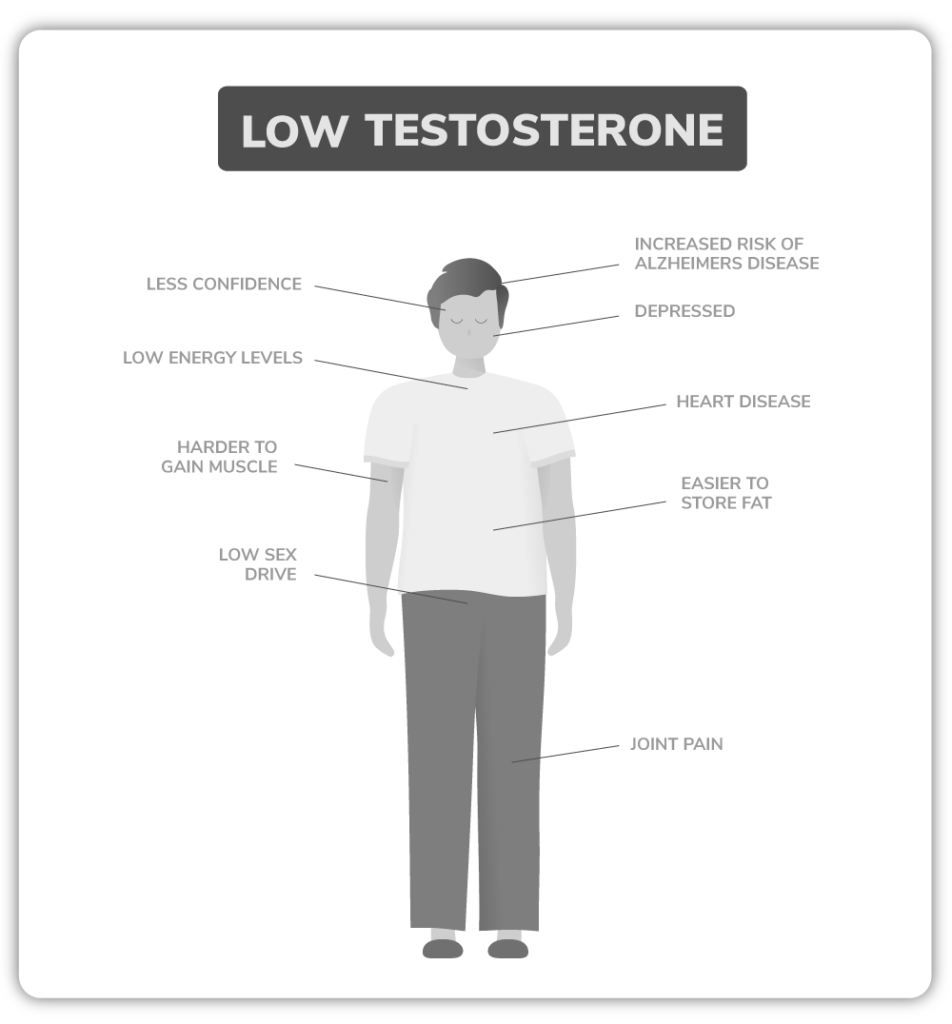
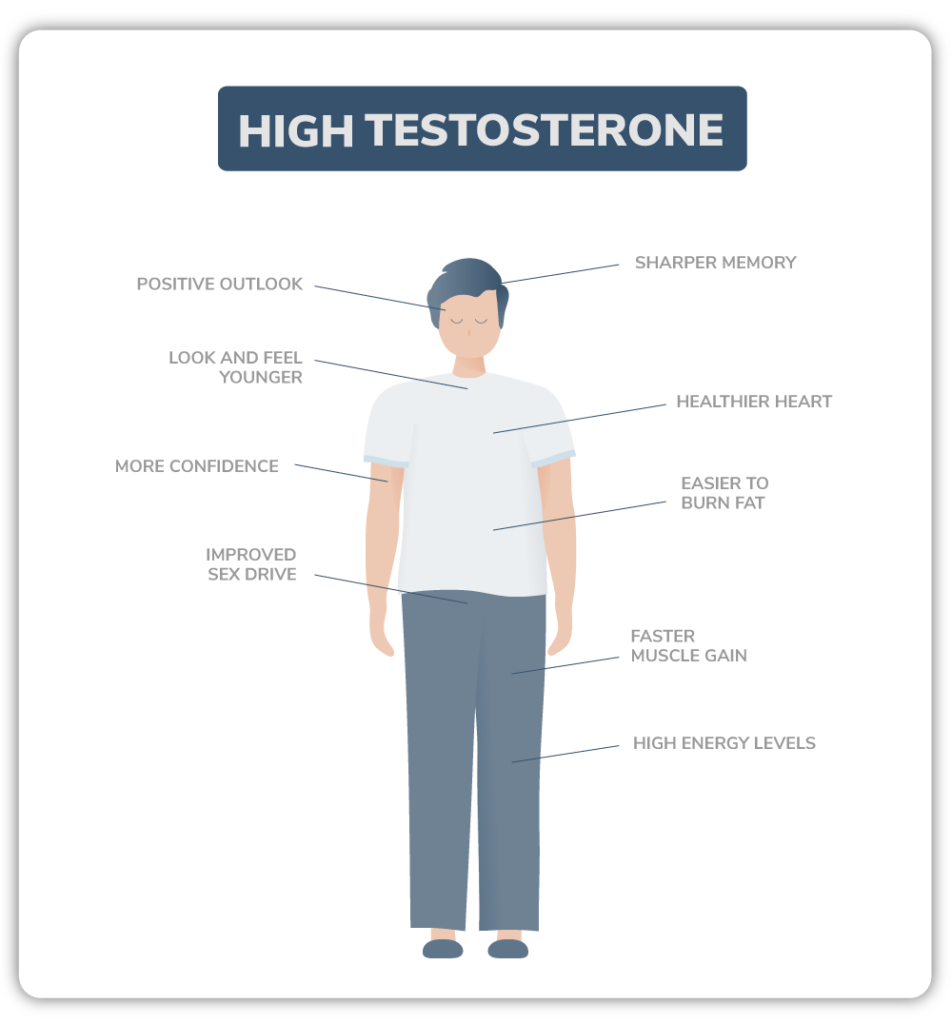
Low levels of androgens in the blood can produce characteristic and indicative signs and symptoms, within which there are:
- Small or underdeveloped testicles.
- Poor body hair such as beard, chest, armpits or genital area.
- Breast enlargement, similar to female breasts (called gynecomastia).
- Difficulty developing muscle mass or weak muscles.
- Fat accumulation usually concentrated in the abdomen, thighs and arms.
- Difficulty in developing and maintaining erections (erectile dysfunction).
- Low sex drive or decreased libido.
- Constant physical fatigue and mental exhaustion.
- Difficulty sleeping properly or insomnia.
- Hot flashes at night (episodes of sudden, uncomfortable heat at night).
- Difficulty in having children.
- Late puberty (after about 14 years of age).
The onset and intensity of symptoms depend on the age of onset of the deficiency, the length and severity of the decline in blood testosterone levels.
The latter factor (blood testosterone levels) is one of the most relevant.
The European Association of Urology (or EAU) states that normal levels of total blood testosterone should be between 280 and 1,100 ng per dL.


 Yes, this is because prolonged drops in testosterone also affect negatively sex-related emotional responses. As the libido decreases, it becomes more difficult to achieve and maintain effective penile erections that allow for a full sex life.
Yes, this is because prolonged drops in testosterone also affect negatively sex-related emotional responses. As the libido decreases, it becomes more difficult to achieve and maintain effective penile erections that allow for a full sex life.
Andromedi pertenece a las organizciones médicas más destacadas en el sector de la Uro-Andrología