Prostate problems
TREATMENTS for Prostate Problems
Prostate cancer
Prostate cancer is the most common type of malignant tumour in men over 55 years of age worldwide. Four percent of men aged 31-40 years suffer from it. The probability of having prostate cancer rises to 50% in men aged 51-60 years and 80% in men over 80 years of age
- VIDEO: Prostate cancer: laparoscopic surgery (in Spanish)
Prostate cancer
Table of content
- VIDEO: Prostate cancer: laparoscopic surgery (in Spanish)
Chances of developing prostate cancer
Introduction to prostate tumours
According to the American Urological Association (AUA) and multiple institutions around the world, prostate cancer is the most common type of malignant tumor in men over 55 years of age worldwide.
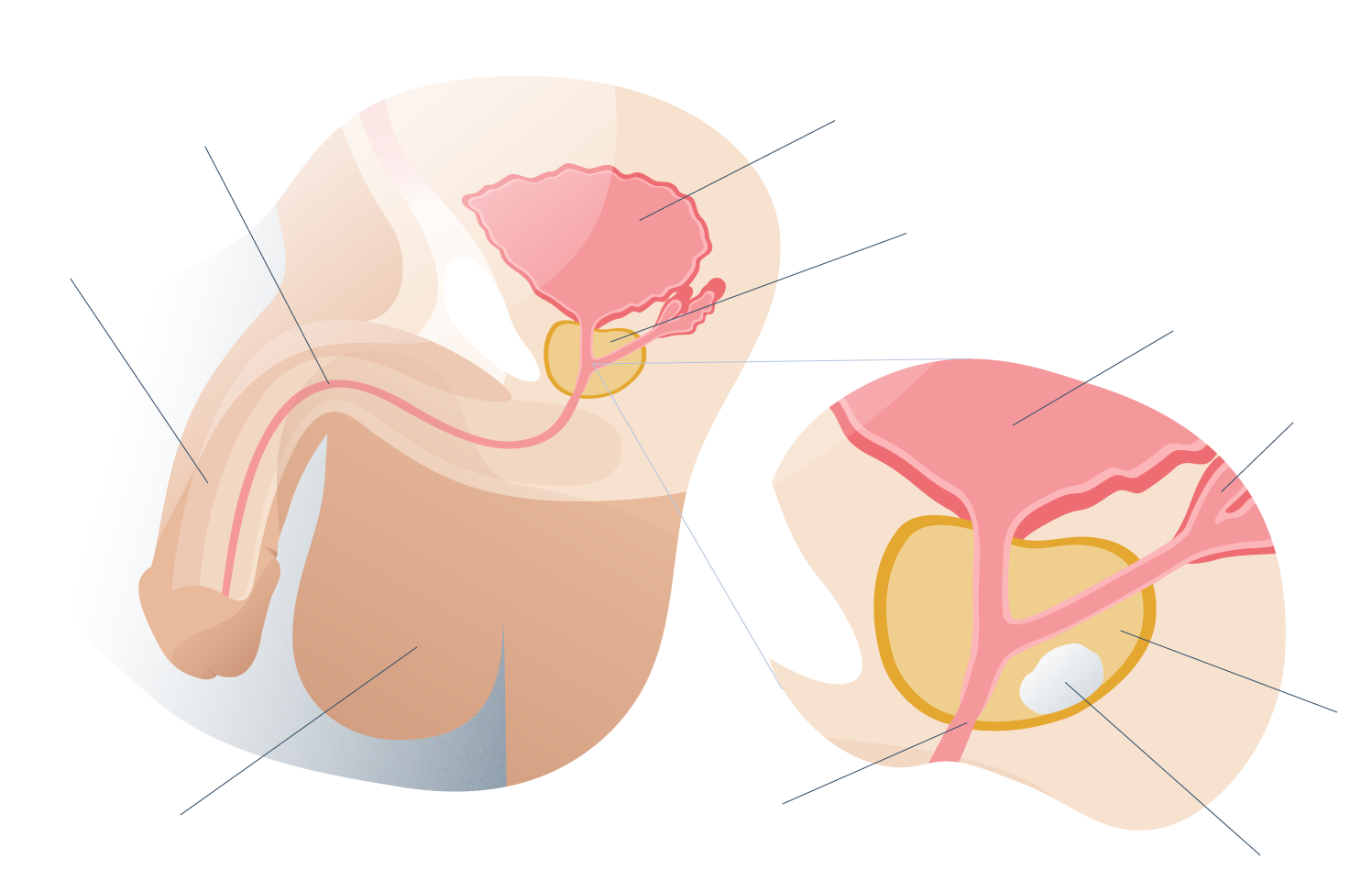
General anatomy of the prostate
In fact, studies show that the prevalence of prostate cancer is higher than is believed. 4% of men between 31 and 40 years old suffer from it, but as the aging process arrives, the probability of having prostate cancer shoots up to 50% in men between 51 and 60 years old and 80% of the elderly 80 years old.
The reasons why this occurs are still unknown, but apparently, age, genetic predisposition (parents or siblings with prostate cancer) and the presence of certain risk factors seem to have a strong relationship.
However, one of the main determinants of the development and worsening of prostate tumors is that a large number of men do not attend urological consultations after 45 years of age because they do not present symptoms and for that reason, the most cases are detected in advanced stages, which complicates the treatment and prognosis of the patient.
If prostate cancer is not treated effectively it can not only affect the quality of life of the patient but also put his own life at risk. The worst complication of this disease is metastasis, in which cancer cells originating in the prostate travel through the body and creates new malignant tumors.
It is important to understand that, although prostate cancer has a truly worrying prevalence, currently available treatments significantly improve patient survival if diagnosis is made early.
Looking for prices and information?
Use our virtual assistant and receive in your email everything related to the treatments that interest you. Budgets, recovery times, hospitalization, financing possibilities month by month, etc.
In just a few minutes and without any commitment.
En cumplimiento del Reglamento General de Protección de Datos le informamos que los datos por Vd. proporcionados serán objeto de tratamiento por parte de Andromedi con la finalidad de prestarle el servicio solicitado y/o contratado. Los datos no se cederán a terceros salvo en los casos en que exista una obligación legal. Para más información puede consultarla pinchando aquí.

TREATMENTS
Is prostate cancer treated?

Yes. Prostate cancer is not a definitive diagnosis and, increasingly, the therapeutic options are greater and with better levels of safety and efficacy.
After having confirmed the presence of cancer and location, size and stage of development of the tumor, we proceed with treatment that is usually comprehensive to increase the chances of recovery.
Depending on the severity of the cancer, the urologist or specialist in urological oncology indicates the correct treatment and through special tests they are evaluated over time.
Generally, cancer treatments (including prostate cancer) are adapted to the type of tumor and the evolution of the patient, but if they are ineffective it is possible to combine them with each other or move on to more radical therapeutic options such as surgery, which usually has excellent results in most cases.
How do you choose the ideal medical treatment?
In some cases, prostate cancer can develop so slowly that it reaches a point where it does not grow any more, but it is almost always necessary to resort to different treatments and reverse the growth of the tumor and prevent complications.
Each case is completely different from the others and must be carefully evaluated by the treating physicians with the absolute collaboration of the patient.
The initial treatment plan depends, among other things, on the following factors:
Info
Which is evaluated using scales such as the Gleason system or the TNM staging system (which refers to the status of the tumor, the lymph nodes and the presence or absence of metastases).
Obviously, if the patient has signs or symptoms of carcinogenic processes in other parts of the body, prostate cancer should be considered as high risk and immediately start with a comprehensive treatment plan.
Chronic diseases such as diabetes (among many others) and poor health habits tend to complicate treatment and it is necessary to assess certain risks.
The patient's opinion is important, as well as her concerns or doubts before, during and after the application of the treatment. The patient has the right to know the side effects in the short and medium term, the therapeutic options available and the objectives of each treatment.
With which it is possible to evaluate the tumor and examine whether it has spread to neighboring nodes or organs. Imaging tests also help predict whether the tumor may come back after treatment (this is rare but can happen).
Active surveillance
The main objective of active surveillance is to continuously evaluate the prostate tumor through imaging tests such as MRI, digital rectal examination, and blood tests to determine the levels of prostate specific antigen (APE), a substance that is elevated in the plasma of men with malignant tumors of the prostate.
Active surveillance is not a proper treatment, but it is part of any type of prostate cancer therapy. In fact, active surveillance can help the doctor see if the cancer has grown or spread and thus change treatment or include new procedures.
Pros and cons of active surveillance
This medical management for prostate cancer is only useful in very small, well-defined tumors with a low risk of growing or spreading to other tissues and in which there are few obstructive symptoms in the urine. Active surveillance can help delay more aggressive treatments and biopsies. However, if the tumor grows, it is necessary to evaluate the possibility of surgery or other types of treatments and for this, the patient must periodically attend urological consultations.
Tumor-directed therapy
Surgery
Surgical treatment is the only completely definitive solution in cases of well-localized tumors without invasion of other organs or tissues. There are many variants of surgeries for advanced prostate cancer or prostate resistant to some traditional treatment, but in general terms, they are known as prostatectomies.
Traditionally, prostatectomies were performed through open surgery, but eventually some more modern and much safer methods replaced it. An example of this is laparoscopic prostatectomy, which has better results, faster recoveries, and minimal side effects.
Laparoscopic prostatectomy aims to remove the prostate or part of it depending on the extent of the cancer using laparoscopic methods. Some small incisions are made in the abdomen of the patient through which the surgical instruments are inserted, which, operated by a surgeon, reach the gland and carefully cut its joints and remove it.
The surgeon then reconnects the ends of the urinary urethra and closes the incisions in the abdomen. The patient must stay in the hospital for a few days and then keep postoperative appointments.
Robotic surgery is also an excellent, safe, and effective option for removing prostate tumors.
Radiotherapy
Radiation therapy consists of applying high-energy rays to the tumor to slow the growth and division of cancer cells or better yet, induce their death. In some cases, radiation therapy may be the only treatment for prostate cancer or it may be an adjunct to other treatment options, such as when the tumor reappears after surgery (which is rare).
The energy used by radiation therapy to destroy the prostate tumor consists of a specialized instrument that emits a fine beam of charged photons with a low radiation mass. Radiation doses can vary according to the needs of the tumor.
There are two main types of radiation therapy. The first of these is external beam radiotherapy, which consists of an x-ray emitting device but it has many disadvantages since it is difficult to focus the rays and some nearby tissues can be affected. The other type of radiation therapy is known as brachytherapy (or internal radiation) and is safer than the previous one. This consists of introducing a small chemical particle through a hollow needle that releases radiation into the surrounding tissue and kills cancer cells.
Radiation therapy is a less invasive procedure than surgery but is only helpful in the early stages of prostate cancer. In addition, radiation therapy can leave side effects such as urinary incontinence, gastrointestinal problems, and erectile dysfunction. Hormone therapy combined with radiation therapy can cause osteoporosis and a tendency to bone fractures.
Cryotherapy
Cryotherapy is an effective treatment with minimal risk in the early stages of tumor development and consists of applying, by means of a thin needle, cold that leads to freezing and destruction of the tissue. It is done under general anesthesia and lasts less than an hour.
The freezing needle (or cryoprobe) is placed inside the tumor under ultrasound guidance. This procedure is applied in patients with prostate cancer in whom it is impossible to perform surgery or apply radiotherapy due to other health problems.
High intensity focused ultrasound
Better known as HIFU by its acronym in English, high intensity ultrasound uses energy in the form of high frequency sound waves to raise the temperature of the affected prostate tissue and induce, in this way, the death of cancer cells. A patient with localized prostate cancer may be a candidate for this treatment.
In this case, the instrument that emits ultrasound into the gland is located by an MRI. This ensures that tissue destruction is done in a controlled manner.
"Prostate cancer is treatable. It is not a definitive diagnosis and increasingly, the therapeutic options are greater and with better levels of safety and efficacy."
Systemic therapy
Chemotherapy
Chemotherapy treatment is the therapeutic method indicated in advanced cases of prostate cancer and is based on the administration of drugs capable of destroying cancer cells in any part of the body, including those of this male gland. Chemotherapy is also used when cancer has spread throughout the body, a phenomenon known as metastasis.
However, the drugs given in chemotherapy treatment have too many side effects since it is impossible to distinguish between cancer cells and healthy cells. Therefore, the types of chemotherapy, the doses and the frequency of administration of these drugs are carefully monitored.
The most common side effects from chemotherapy are constant fatigue, loss of appetite, nausea and vomiting, hair loss, diarrhea, and an increased risk of anemia or infections.
Immune therapy
Immune therapy (or immunotherapy) stimulates the body’s defense mechanisms to attack prostate cancer cells. They tend to have very few side effects and are very safe.
However, most variants of cancer immunotherapy are still in clinical trials and their work is not always effective in all patients.
Hormonal therapy
Testosterone, the main male hormone, plays a fundamental role in the development of prostate cancer in men with a predisposition to this disease. Cancer cells of the prostate require testosterone to divide and hormonal treatment aims to inhibit this mechanism.
Hormone therapy helps to deprive cancer cells of the dissolved testosterone in the blood and as a result, tumor growth stops and, in the best case, reverses naturally. Obviously, this type of treatment is useful only in the initial stages of the disease, when the tumor is still growing and has not spread to other organs.
Hormone therapy for prostate cancer is known as androgen deprivation therapy (APT) and is often used in combination with other treatments such as surgery or chemotherapy.
The big problem with androgen deprivation therapy is that it has many side effects and in the long term, cancer cells develop the ability to evade these drugs. Hormone therapy resistant prostate cancer must be managed with more aggressive treatments.
Other tips during treatment
In addition to complying with all the medical indications, going to a urological or oncological consultation periodically and receiving treatment (or a combination of them), the patient must take into account certain tips that will not only help them feel better but will most likely improve their disease prognosis.
Some of these tips are:
- Maintain a balanced diet: Low in fat and ultra-processed foods such as flour or junk food, as well as reducing the consumption of salt and foods with a high content of preservatives or chemical dyes. Increasing the consumption of vegetables and fruit juices provides minerals and energy for the cells of the immune system (which are always trying to destroy cancer cells).
- Stay hydrated by drinking at least 8 glasses of water a day (this includes fruit juices). Drinks such as coffee, soda, and energizers can promote dehydration and make the patient feel fatigued.
- Practicing physical exercise optimizes immune function, maintains muscle mass and joints in optimal condition, improves mood and general health. The ideal is 30 minutes a day of light exercise or some weight lifting (as long as the patient's health conditions do not prevent it).
- Maintain an adequate weight: because overweight or obese patients tend to have poorer prognoses compared to those who have an ideal weight. Dyslipidemias (excess fats in the blood) appear to promote the growth and division of cancer cells
- Avoiding smoking not only improves respiratory function but also favors the state of well-being in the body. Nicotine and other chemicals in tobacco are carcinogenic.
- Take care of mental health. Prostate cancer patients often fall into depression or begin to experience intense episodes of anxiety and nervous stress. Psychological therapy and other self-care tools such as meditation, sports, rest, or simply sharing with friends or family can significantly help in recovery.
What is the survival rate in prostate cancer?
The vast majority of patients with prostate cancer do not die from this disease but naturally from others. Thanks to scientific advances and current novel treatments, prostate cancer is no longer a definitive diagnosis.
In fact, the survival rate for prostate cancer is 95% five years after diagnosis and starting treatment. This type of cancer usually grows very slowly, which allows early detection if the patient begins urological consultations around 50 years of age.
"The survival rate for prostate cancer is 95% five years after diagnosis and initiation of treatment."
Summary of treatment
Prostate cancer. What is it?
It is a disease characterized by the presence of a malignant tumor with cancer cells within the glandular portion of the prostate, a male gland located below the urinary bladder. Remember to visit us at our Andromedi centres in Madrid, Seville or Tenerife for more information.
Causes
Risk factors for prostate cancer can be many, among which are genetic predisposition, being of African descent, being over 50 years of age, smoking, a diet high in fat and physical inactivity.
Diagnosis
The diagnosis of prostate cancer consists of digital rectal examination, blood tests to measure the concentration of prostate specific antigen, ultrasound, MRI, and tissue biopsies to visualize the cancerous characteristics of the cells.
Treatment
The clinical management of this disease depends on the stage of development of the malignant tumor and this treatment can range from less radical measures such as pharmacotherapy, hormonal therapy or immunotherapy to surgery to remove the prostate.
Symptom
Because it is a (malignant) prostate enlargement, this type of cancer causes signs of obstructive obstruction in the urinary flow in the intermediate and severe stages of the disease. Difficulty urinating or obstruction cComplete may indicate a problem.
Complications
If prostate cancer is not treated in a timely manner with the correct therapy, it is possible that the prostate enlargement generates a total obstruction of the urine and a considerable risk of metastasis is reached, especially in the bones and lungs.
Surgical procedure
What is prostate cancer?
Prostate cancer is a common disease in older men and occurs when a malignant tumor develops somewhere in the gland. The cells of the prostate begin to reproduce rapidly and grow in size, therefore obstructions in the urinary tract occur.
Prostate growths can be of two types: benign and malignant.
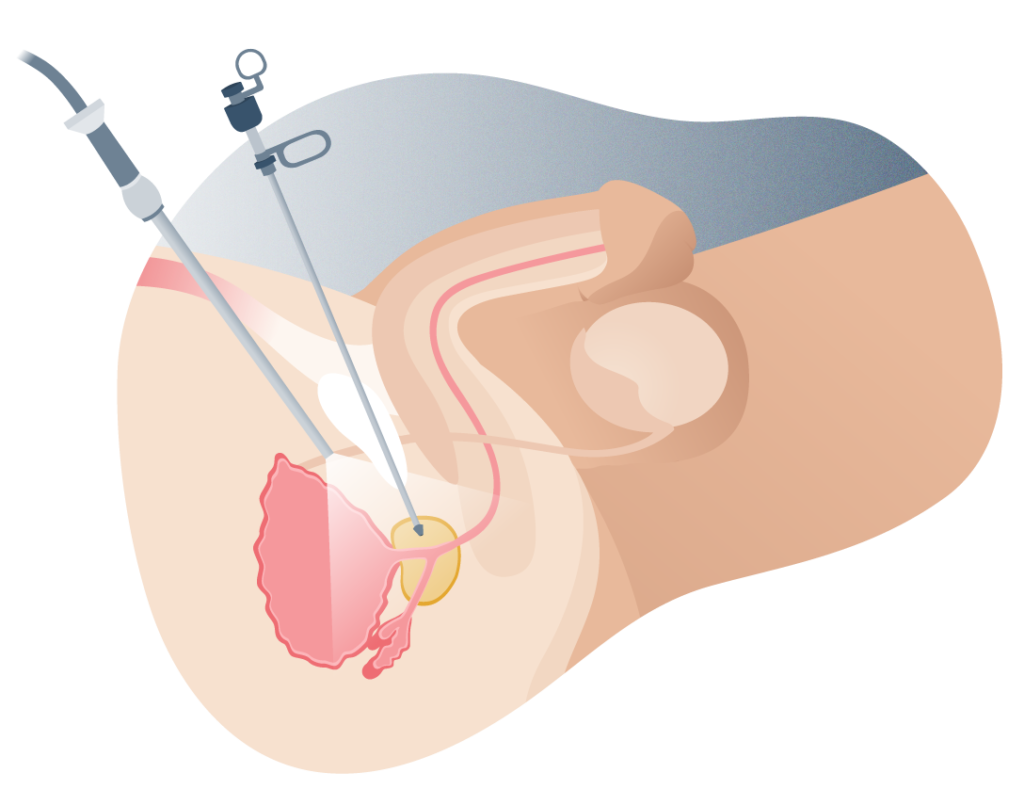
TUR trans urethral resection of the prostate
"In our centres in Madrid, Seville or the Canary Islands (Tenerife), we carry out the techniques and treatments with the most modern facilities and the best specialists and equipment to guarantee an effective solution".
Benign prostatic enlargements are known as benign prostatic hyperplasia and are characterized by:
- They are not a risk to the life of the patient.
- They stay in the prostate and do not affect other tissues in the body.
- They can be removed by surgery and do not grow back (or do so very slowly).
On the other hand, malignant prostate growths called prostate cancer tumors are characterized by:
- Represent a serious threat to the life of the patient.
- They have the ability to invade other organs and tissues of the body (metastasis).
- They can be removed by surgery but can grow again (some cancer cells will always remain inside the prostate unless it is completely removed).
Anatomy and function of the prostate
The prostate is a male gland that is small in size, similar to a walnut and is located below the urinary bladder, surrounding the urethra that carries urine from this reservoir (the bladder) to the penis.
Prostatic secretion contributes to the volume of semen that is ejaculated during arousal, whose main function is to nourish and protect the sperm produced in the testicles. The normal prostate functions under nervous and hormonal control.
In addition, the prostate has the function of acting as a pump that drives the semen during ejaculation and prevents this fluid from going to the bladder (this disorder is known as retrograde ejaculation).
What factors favor the development of prostate cancer?
The causes of prostate cancer remain a mystery and there is still great interest in scientific research as some men develop this disease while others do not.
The main risk factors for prostate cancer are.
Info
The risk of developing prostate cancer increases with aging and in fact, cases of this disease in men under 40 years of age are really rare. The own risk due to advanced age increases if the patient has other risk factors.
For some genetic reason, African American (or black) men tend to have a higher prevalence of prostate cancer and in more severe degrees. However, Caucasians, Hispanics, or Asians are also affected.
Having (or having had) a father, grandparents or siblings with prostate cancer increases the risk 2 or 3 times than those individuals without cases of this type of tumors in their family.
Evidence shows that consuming animal fats, refined sugar, and processed foods increases the risk of developing prostate cancer. A balanced diet can reduce the risk of this disease.
Little physical activity added to overweight conditions increases the risk and severity of prostate cancer.
Or pipe smokers have twice the risk of prostate cancer compared to those who do not.
Las prostatectomías
Las prostatectomías son cirugías complejas que requieren un alto nivel de precisión técnica ya que se realiza una extirpación total (o casi total) de la próstata y los tejidos que la rondan, como algunos ganglios linfáticos o las vesículas seminales si existe diseminación de células cancerígenas en esta zona, pero el gran dilema son las estructuras no implicadas en el cáncer que podrían ser lesionadas con la intervención como los nervios eréctiles.
Las prostatectomías
Las prostatectomías son cirugías complejas que requieren un alto nivel de precisión técnica ya que se realiza una extirpación total (o casi total) de la próstata y los tejidos que la rondan, como algunos ganglios linfáticos o las vesículas seminales si existe diseminación de células cancerígenas en esta zona, pero el gran dilema son las estructuras no implicadas en el cáncer que podrían ser lesionadas con la intervención como los nervios eréctiles.
La resección transuretral de la próstata consiste en:
1 Introducir el extremo libre del resectoscopio en la uretra desde la punta del pene.
2 La punta del resectoscopio se ubica a nivel de la uretra prostática y se comienza a cortar el exceso de tejido.
3 Las porciones grandes de tejido son presionadas con pinzas especiales en el resectoscopio y se halan hacia afuera. Si son muy pequeñas, pueden atravesar el esfínter de la vejiga y quedarse ahí hasta que el paciente las orine.
4 El cirujano urólogo retirará el resectoscopio y se introducirá una sonda vesical durante algunos días (generalmente menos de 48 horas).
Signs and symptoms
Signs and symptoms of prostate cancer
In the initial stages of the disease, generally, the asymptomatic patient does not know that he has a problem and for this reason, urological evaluations are delayed. However, if the tumor grows inside this organ, life is endangered and some symptoms appear such as:
- Presence of blood in the urine, especially if there is no pain.
- Difficulty starting to urinate..
- A weak or intermittent stream of urine.
- Feeling of not having emptied the bladder after urinating
- Bone pain or bone fractures (indicates metastasis).
Why does BPH cause so many problems?
The prostate is a gland located around the urethra, just below the sphincter of the urinary bladder. If the prostate becomes inflamed, the tissue growth is concentric, i.e. towards the urethra.
When the urethra is compressed and urine is obstructed, the bladder overflows its storage capacity and incontinence (when the pressure within the bladder is so great that it passes through the prostatic compression site into the urethra) or a kidney problem known as hydronephrosis, in the worst case, can occur.
Incomplete emptying of the bladder can predispose to urinary tract infections and kidney stones (commonly known as renal lithiasis).
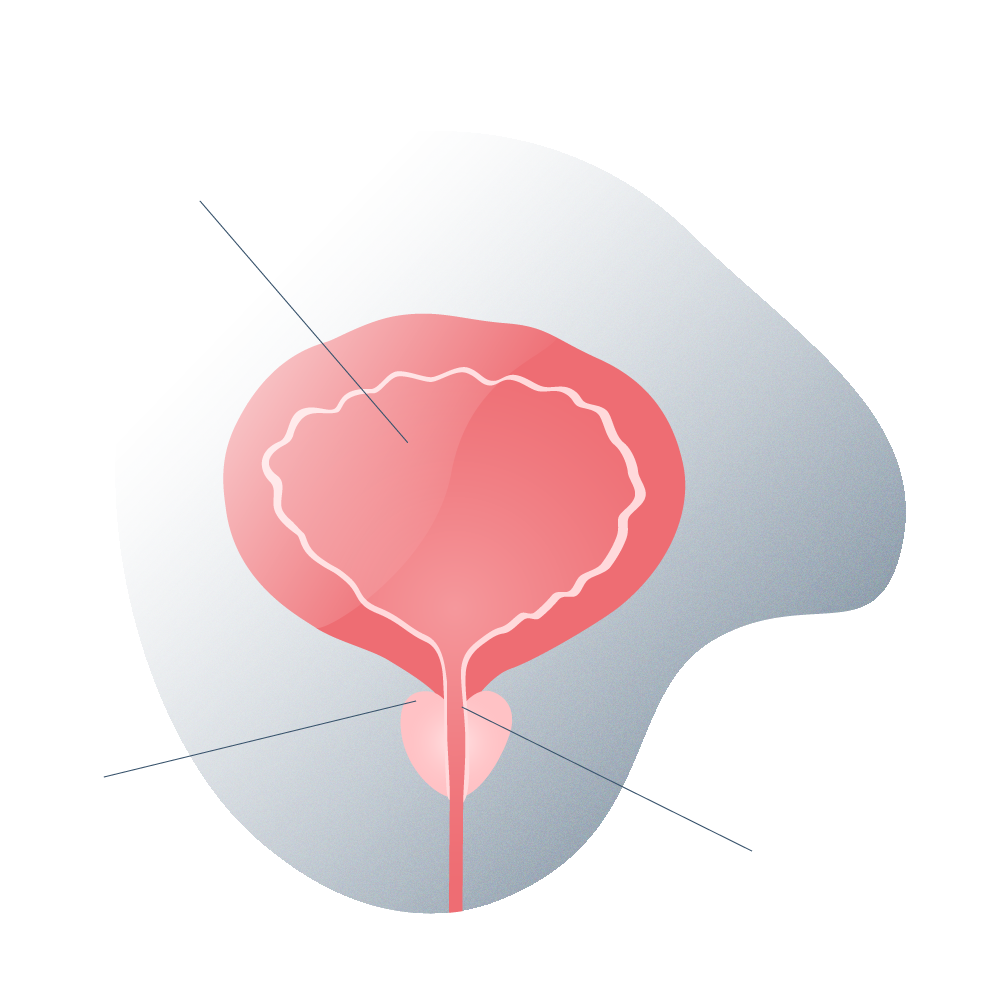
Healthy prostate

Prostate with inflammation
Complications
It should be noted that complications from prostate cancer are reached in advanced stages of the disease and are generally:
- Metastasis, especially in the lungs and bones.
- Erectile dysfunction or the inability to have hard, long-lasting erections.
- Recurrence of cancer after treatment.
- Death (it is the second cause of death It is due to cancer in men in countries such as the USA or the European Union).
Most patients receive a timely diagnosis and effective treatment, so the complication rate is low in developed countries such as Spain.
"Most patients receive timely diagnosis and effective treatment, so the complication rate is low in developed countries such as Spain".
How it is diagnosed
Diagnosis of prostate cancer
Early detection is key to finding the ideal treatment, within all treatment options. In addition to the correct physical examination and anamnesis (or medical interview), prostate cancer requires other methods to be confirmed, for example:
Info
Which consists of inserting a doctor's finger through the anus to feel the gland and evaluate if it is enlarged. It is an easy, fast and safe method.
This substance is considered a tumor marker since it increases its concentration in the blood if there is a cancer process in the prostate.
Which is performed only if there are suspicions of prostate tumors and consists of removing a small amount of tissue from the prostate to observe it under a microscope. With a biopsy, it is possible to determine the types of cancers found in a tissue sample.
Your doctor will likely order some imaging tests such as ultrasounds, CT scans, or MRIs.
What are the stages of prostate cancer?
The system used by urologists to classify malignant tumors of the prostate is known as TNM and takes into account the status of the tumor itself (its size, location, whether there are several tumors or is it only one), the status of the tumors. Lymph nodes in the inguinal area and whether or not there is metastasis.
Análisis de orina
Los análisis de orina sirven para determinar la química de esta sustancia, la función renal y la existencia o no de agentes patógenos causantes de una infección.
A menudo, la hiperplasia benigna de próstata puede producir retención de orina en la vejiga y aumentar el riesgo de infecciones, especialmente en pacientes diabéticos o con problemas inmunológicos.


Pruebas de imagen (urografía y ecografía pélvica)
Las pruebas de imagen permiten evaluar de manera más precisa la obstrucción de la uretra prostática. Las principales pruebas son la urografía y la ecografía.
La urografía consiste en inyectar una sustancia que, una vez filtrada por los riñones y dispersada en la orina, se pueden realizar radiografías especiales para poner en evidencia el contorno de la vejiga y la uretra. El sitio de estrechez uretral se ubica fácilmente.
La ecografía es una prueba rápida y económica que consiste en un aparato que crea imágenes bidimensionales de las estructuras internas como la vejiga (que debe estar llena de orina) al emitir ondas de ultrasonido. Es completamente indoloro y no se emite radiación ionizante (como es el caso de la urografía).

Frequently asked questions
Frequently asked questions at the Andromedi centres in Madrid, Seville and Tenerife
In the best of cases, a malignant tumor in the prostate can encapsulate but this happens very little. Untreated tumors tend not only to grow out of control but to multiply in other organs of the body. In addition, an enlarged prostate can cause obstruction of the urine.
It is likely that during prostatectomy some nerves to the penis are accidentally cut, leaving it without part of its innervation and with difficulties in inducing an erection naturally. This only happens in less than 25% of cases but it is a risk that is run, however, erectile dysfunction has a solution.
Yes, and indeed, physical therapy can help improve urinary function after prostate removal surgery. The physical therapies with the best results in this area are Kegel exercises and neuromuscular electrical stimulation, which strengthen the pelvic floor muscles. Certain positive effects on sexual function are also achieved with these procedures.
The existence of risk factors predisposes to the development of this disease and healthy practices that help maintain heart health can also prevent and decrease the severity of prostate cancer. These healthy habits include a healthy diet, physical exercise, and avoiding tobacco use, among others. Routine check-ups with the urologist are essential for early diagnosis.
Each case is evaluated individually but if the prostate cancer has metastasized, the patient should receive chemotherapy combined with hormonal therapy. The prognosis of the disease is usually reserved in these cases and professional monitoring and the patient's family members are required.
There is no reliable evidence to support the hypothesis that benign prostatic hyperplasia (a common diagnosis in men over 40 years of age) turns into cancer. However, both conditions usually produce similar symptoms and can be quickly detected by digital rectal examination.
Medical references and bibliography
- Prostate cancer Spanish Society of Medical Oncology
- Prostate cancer MSD Manual for Professionals in Spanish
- What is prostate cancer? (in Spanish) Institute for Cancer of USA
- Are you at risk? (en inglés) Prostate Cancer UK
- How Is Prostate Cancer Diagnosed? CDC – USA
- Relation between diabetes and BPH PubMed
- Diagnosis of prostate cancer National Library of Medicine
- Prostate Cancer: Treatment National Health System of UK
- Prostatectomy Mayo Clinic
Author
Andromedi pertenece a las organizciones médicas más destacadas en el sector de la Uro-Andrología